Diagnosing obstructive sleep apnea (OSA) begins with distinguishing simple snoring from breathing interruptions that occur during sleep. Because symptoms are not always noticeable to the patient, evaluation typically includes screening questionnaires and a sleep study. Sleep testing—performed either in a laboratory or at home—monitors breathing patterns, oxygen levels, heart rate, and sleep stages to measure the severity of apnea using the respiratory disturbance index (RDI). In some cases, additional testing such as sleep endoscopy may be needed to identify the exact anatomical source of airway obstruction and guide appropriate treatment.
 Knowing the difference between simple snoring and sleep apnea is key to effective treatment. While snoring results from the relaxed tissues in the throat blocking the airway partially, sleep apnea involves frequent, loud snoring combined with a cessation of breathing. The best way to determine if a patient has OSA is through a sleep study in which breathing and other body functions are monitored overnight. Screening questionnaires which are often used to determine if a patient requires a sleep study are:
Knowing the difference between simple snoring and sleep apnea is key to effective treatment. While snoring results from the relaxed tissues in the throat blocking the airway partially, sleep apnea involves frequent, loud snoring combined with a cessation of breathing. The best way to determine if a patient has OSA is through a sleep study in which breathing and other body functions are monitored overnight. Screening questionnaires which are often used to determine if a patient requires a sleep study are:
- Epworth Sleepiness Scale: Questionnaire in which a patient rates the chances of falling asleep in various situations. The scale is used to assess the patient’s daytime sleepiness levels from supernormal to dangerously sleepy.
- The Rome Questionnaire: A 7 item questionnaire which is used in conjunction with Body Mass Index (BMI) to identify a patient’s risk of OSA.
During sleep testing, the persistence and loudness of snoring are typically recorded, as well as body position and the sleep phases in which the snoring occurs. Common sleep studies include:
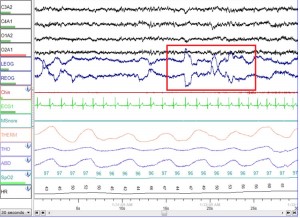 Nocturnal polysomnography: While the patient sleeps, equipment monitors breathing patterns, heart, lung, and brain activity, leg and arm movement, and blood oxygen levels. The polysomnography reports the respiratory disturbance index (RDI), which is the number of apneas or hypopneas lasting 10 seconds or more per hour of sleep. A patient with an RDI of 5 or less is considered a simple snorer with no OSA. An RDI of 5-15 suggests mild OSA, 16-30 indicates moderate OSA, and more than 30 indicates severe OSA.
Nocturnal polysomnography: While the patient sleeps, equipment monitors breathing patterns, heart, lung, and brain activity, leg and arm movement, and blood oxygen levels. The polysomnography reports the respiratory disturbance index (RDI), which is the number of apneas or hypopneas lasting 10 seconds or more per hour of sleep. A patient with an RDI of 5 or less is considered a simple snorer with no OSA. An RDI of 5-15 suggests mild OSA, 16-30 indicates moderate OSA, and more than 30 indicates severe OSA.- Home Sleep Test: A simpler test using portable monitoring devices to measure heart rate, blood oxygen level, and airflow and breathing patterns.
Types of ambulatory monitors your doctor may recommend:
- Eden Trace: Monitors oxygen saturation, chest wall impedance, nasal and oral airflow, heart rate, and body movement.
- The Nightwatch System: Records eye, leg, chest and abdominal movement, heart rate, nasal oral airflow, and body position. This system can calculate the patient’s RDI and send 2 minute sections of recordings for lab analysis.
- The MESAM IV System: Analyzes heart rate, snoring, and saturation change to determine sleep disordered breathing.
- WatchPAT200: The peripheral arterial tonometer (PAT) is a wrist worn device which detects obstructive occurrences.
In some cases, a sleep endoscopy may be required to determine what is obstructing the upper airway, especially if a blockage in the nose or throat is suspected.
If you have any issues with snoring or possibly obstructive sleep apnea, schedule an appointment with one of our physicians at Fort Worth ENT & Sinus. Please complete an online appointment request or phone 817-332-8848.
Frequently Asked Questions
Occasional snoring is common and often harmless. However, loud, chronic snoring combined with choking sounds, gasping for air, or long pauses in breathing may indicate obstructive sleep apnea. Excessive daytime sleepiness, morning headaches, and difficulty concentrating are also warning signs that warrant evaluation.
Yes. Many people with obstructive sleep apnea are unaware of their symptoms, especially if they sleep alone. Even without noticeable daytime fatigue, untreated OSA can increase the risk of high blood pressure, heart disease, stroke, and diabetes. A sleep study provides objective data to confirm or rule out the condition.
Home sleep tests are effective for diagnosing many cases of moderate to severe obstructive sleep apnea and are more convenient for some patients. However, in-lab polysomnography remains the most comprehensive option, particularly for patients with complex symptoms, other sleep disorders, or unclear home test results.
Mild obstructive sleep apnea does not always require aggressive treatment. Depending on symptoms and overall health, management may include lifestyle changes, positional therapy, oral appliances, or close monitoring. Your physician will recommend a treatment plan tailored to your specific needs.
A sleep endoscopy may be recommended if the exact location of airway obstruction is unclear or if surgical treatment is being considered. This procedure allows the physician to directly visualize how the airway collapses during sleep, helping guide more precise and effective treatment decisions.


